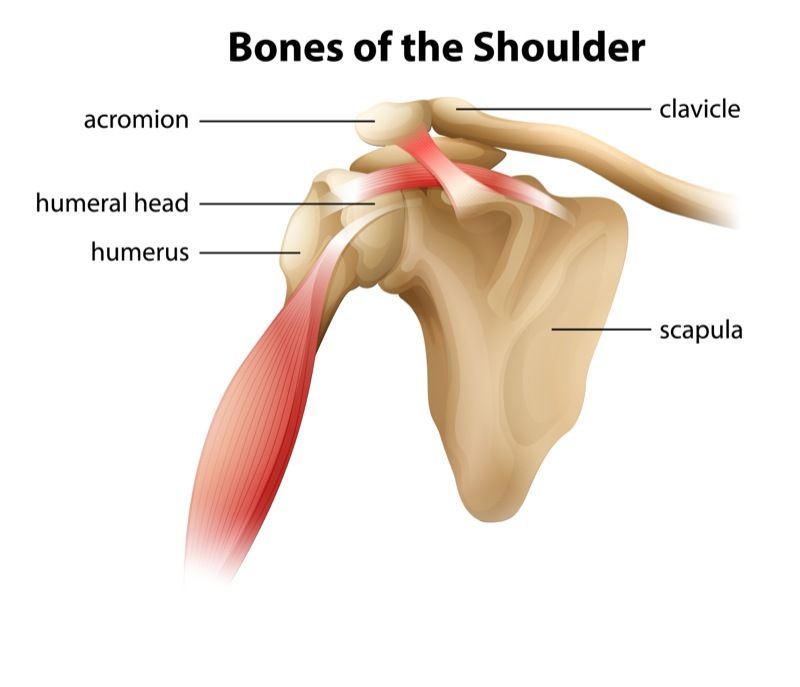
Protect the injection site for a day or two. For example, if you received a cortisone shot in your shoulder, avoid heavy or repetitive overhead lifting for 24 to 48 hours.
It is normal to have some increased discomfort in the injected site for the first 24 to 48 hours. Apply ice to the injection site 20 minutes at a time, 3 to 4 times a day as needed to relieve pain. Heat is generally not helpful in relieving the discomfort from the injection as it increases the inflammatory response.
For injection site soreness during the initial 24-48 hours, you may take the pain reliever acetaminophen (Tylenol). Limit this to a total of 3000 mg throughout 24 hours, and do not take it if you have liver disease. You may also take an anti-inflammatory such as Aleve, Advil, Motrin, or Ibuprofen if you are not taking a blood thinner (Plavix, Coumadin, Eliquis, etc.), do not have bleeding tendencies, ulcers, acid reflux, etc., and you are not already taking other anti-inflammatory medications such as Meloxicam (Mobic), Celebrex (Celecoxib), Piroxicam (Feldene), etc. If you have any concerns, please talk to your orthopedic surgeon or primary care physician before taking these medications.
Watch for signs of infection such as increasing pain, redness, and swelling lasting more than 48 hours. If you notice any signs of infection following your joint injection (fever greater than 101.5 degrees, redness, warmth, drainage), call OrthoMed’s office immediately at (209) 524-4438.
You may shower immediately after the injection but do not soak in a bathtub, hot tub, or whirlpool for 48 hours.